What Is Celiac Disease? Causes, Symptoms And Treatment
author parentcircle author parentcircle author parentcircle author parentcircle author parentcircle author parentcircle
Worried that your child may have symptoms of celiac disease? Read on to know what causes celiac disease, its symptoms in kids, its complications and the treatment options.
Are you concerned about your child having frequent bouts of vomiting, bloating, diarrhoea or constipation after eating certain foods? Does he seem to be irritable or crying all the time?
If your child is eating well but does not seem to be gaining weight or having other health issues, he may be suffering from symptoms of celiac disease, an autoimmune disorder caused by intolerance to gluten, a protein found in wheat, rye and barley. Recent research indicates that the prevalence of celiac disease is much higher in children when compared to adults.
Here are some FAQs regarding celiac disease which is a worldwide problem with no specific medical treatment available. Read on to know more about the causes of celiac disease, its symptoms and treatment options.
What is celiac disease? Is it the same as gluten sensitivity? If not, what are the differences?
Celiac disease is a serious genetic autoimmune disorder. It is also referred to as celiac sprue, non-tropical sprue, and gluten-sensitive enteropathy. It is a common disorder and its prevalence has been estimated to be about 1 in 100 people worldwide.
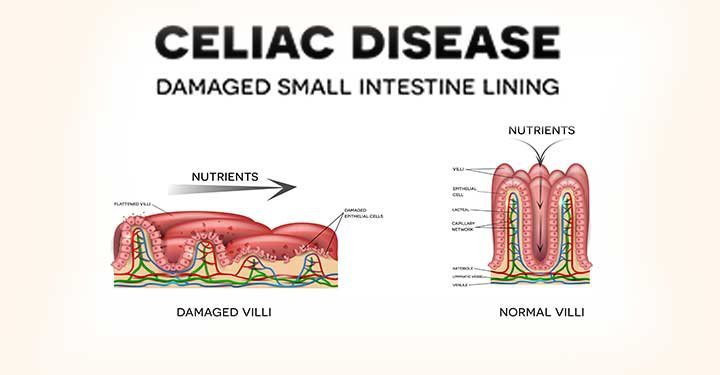
Consuming gluten (a protein which is found in wheat, barley and rye) triggers an immune response in genetically predisposed individuals, where the body mounts an attack on the small intestine and destroys the intestinal villi. The villi are finger-like projections in the lining of the small intestine which aid in nutrient absorption. When the intestinal villi are damaged, it hampers nutrient absorption into the bloodstream leading to other health conditions.
Non-celiac gluten sensitivity (NCGS) is a condition where some people have symptoms of gluten intolerance but do not have celiac disease or allergy to wheat. They have symptoms of mental fatigue, gastric distress, fatigue and headache, all of which can improve with the elimination of gluten from diet.
What are the symptoms of celiac disease?
Diagnosing celiac disease can be difficult as patients may have different symptoms. Also, some patients who have tested positive for celiac disease may be free of any symptoms characteristic of celiac disease. Also, in some instances, those who test positive for celiac disease on a blood test may show negative results on an intestinal biopsy.
Celiac disease symptoms in children
Children usually present with digestive symptoms. Here's a common list of symptoms manifested in children with celiac disease.
- Decreased appetite
- Abdominal bloating and pain
- Chronic diarrhoea
- Vomiting
- Constipation
- Pale, foul-smelling or fatty stool
- Iron-deficiency anaemia
- Weight loss
- Fatigue
- Irritability in mood and behavioural issues
- Dental enamel defects
- Thin bones/frequent fractures
- Delayed growth and puberty
- Short stature
- Failure to thrive
- Attention deficit hyperactivity disorder (ADHD)
Celiac disease symptoms in adults
Adults with celiac disease may have digestive symptoms like constipation, diarrhoea and abdominal bloating. However, adults can also experience symptoms such as:
- Anaemia
- Fatigue/tiredness
- Headaches or migraines
- Anxiety
- Depression
- Irritability
- Mouth ulcers (canker sores)
- Discoloured teeth
- Infertility or frequent miscarriages
- Missed periods
- Itchy bumps on the skin (dermatitis herpetiformis or Duhring's disease)
- Joint pain
- Liver disease
- Poor weight gain
- Thin bones
- Tingling/numbness in hands and feet
What are the complications of celiac disease?
Most of the complications of celiac disease occur due to the long-term effects of malabsorption in the intestine.
- Malnutrition: This is the most common complication of celiac disease. Inability to absorb vital nutrients can lead to conditions such as iron deficiency anaemia, vitamin B12 and folate deficiency anaemia, and osteoporosis. In severe cases, the patient may develop fatigue, dizziness and confusion along with wasting of muscles. In children, it manifests as delayed development and stunted growth.
- Lactose intolerance: In lactose intolerance, the body is unable to digest the natural sugar (lactose) found in dairy products. This is because the small intestine is unable to produce the enzyme lactase which breaks down the lactose. The undigested lactose moves on to the large intestine where bacterial interaction with the lactose leads to symptoms such as bloating, diarrhoea and abdominal discomfort.
- Bone loss: Inappropriate absorption of calcium and vitamin D leads to poor bone density. As a result, the bones become brittle (osteoporosis) and the individual may suffer from bone pain and bone weakness.
- Irritability and depression: An immune reaction to gluten can lead to psychiatric complications such as ADHD, depression and related mood disorders. This is mentioned in a study by Jackson et al, titled, 'Neurologic and Psychiatric Manifestations of Celiac Disease and Gluten Sensitivity', published in the Psychiatric Quarterly in 2012. Also, nutritional deficiency of zinc and vitamin B12 in the serum have been linked to depression.
- Cancer: The risk of developing cancer is slightly higher in people with celiac disease. The types of cancer associated with celiac disease are small bowel cancer, small bowel lymphoma and Hodgkin lymphoma. Generally, being on a gluten-free diet for 3-4 years brings down the risk of developing cancer.
- Dental defects: Calcium malabsorption at the age of seven or younger results in damage to the tooth enamel and dental cavities. Also, delayed dental development can be seen with the slower eruption of permanent teeth.
How is celiac disease diagnosed?
1. Antibody blood tests: An antibody is a protein released by the body's immune system to fight pathogens or disease-causing germs. However, in people with celiac disease, the immune system mistakes gluten to be harmful to the body and releases certain antibodies to attack it. These antibodies are:
- Anti-tissue transglutaminase (tTG)
- Anti-endomysium (EMA)
- Anti-deamidated gliadin peptides (DGP)
Measuring the levels of these antibodies in blood can help diagnose celiac disease. However, blood tests are not enough to make a conclusive celiac disease diagnosis as the results may occasionally be incorrect.
2. Endoscopic biopsy: A biopsy of the small intestine is the only way to confirm if you are suffering from celiac disease and not symptoms of gluten intolerance or wheat allergy. This outpatient procedure is always done by a gastroenterologist and is done under sedation or local anaesthesia.
In this procedure, a long, thin tube called an endoscope is passed through the mouth and stomach into the upper small intestine. Tissue samples from 5-6 areas are taken using instruments passed through the endoscope. These tissue samples are then examined under the microscope to identify damage to the intestinal villi.
Does celiac disease run in families? Can it pass from parents to children?
Celiac disease tends to occur in families. If you have been diagnosed with celiac disease, there is a 1 in 22 chance of your first-degree relatives (parents, children and siblings) developing the condition. For second-degree relatives (aunt, uncle, cousins), the risk of developing celiac disease is 1 in 39.
While the disease itself is not inherited, the risk of developing celiac disease is inherited. Two types of genes are known to be responsible for this - HLA-DQA1 and HLA-DQB1. Celiac disease is caused by the interaction of these genes with other genes and with environmental factors.
Genetic testing: HLA testing can help identify individuals in the family who are at risk of developing celiac disease. In case the gene test is negative, the person need not undergo regular antibody screening for the rest of his life as he will not develop the condition.
Is celiac disease present from birth? Or does it develop later?
Celiac disease is not present at birth, but children with the celiac genes HLA-DQ2 and DQ8 are certainly at risk of developing celiac disease later in life. It's only after gluten-containing foods are introduced at 6-8 months of age that the symptoms of celiac disease start showing up. Also, children with certain conditions like type 1 diabetes, Down's syndrome and IgA deficiency are at a greater risk of developing the condition.
How can parents suspect that their baby may have celiac disease?
Parents can suspect celiac disease, if the baby has poor growth at the time gluten containing foods are introduced in the diet, i.e., at six months of age. In addition, the baby may have gas or bloating symptoms. Older children have other symptoms like diarrhoea, vomiting and constipation.
Antibody blood tests will reveal if your baby has celiac disease or not. If your baby is found to have high levels of antibodies, an endoscopic procedure for tissue biopsy of the small intestine is recommended. A paediatric gastroenterologist performs the procedure with the child under sedation. Based on the findings of the biopsy, a celiac disease diagnosis is confirmed.
In some cases, your baby may develop symptoms due to wheat allergy. This can be identified by conducting blood tests or skin-prick tests to see if wheat antigen is the culprit.
What is the treatment for celiac disease?
Currently, a strict lifelong adherence to a gluten-free lifestyle is the only treatment for celiac disease. There is no medication or therapy available. Being a chronic autoimmune disease, the symptoms never go away but flare up periodically.
In a gluten-free diet, also known as celiac disease diet, only food containing less than 20 parts per million (ppm) of gluten is allowed. This restricts the damage caused to the intestinal villi and allows the symptoms to resolve gradually. Some healthy foods are naturally gluten free. These include vegetables, fruits, meat, poultry, dairy products and fish. There are also a variety of grains including amaranth, millet, corn, sorghum and quinoa that are gluten-free.
In addition, supplementing the celiac disease diet with vitamin B12 and folate can be effective in recovery from depression and anxiety symptoms.
Are there any breakthrough clinical trials on celiac disease treatment?
The results of a new phase 2 clinical trial using nanotechnology has shown that it is possible to induce immune tolerance to gluten in individuals with celiac disease. The technology can have far-reaching implications on the management of celiac disease in the future.
The technology involved in this celiac disease trial is a biodegradable nanoparticle containing gluten (allergen) that indicates to the immune system that the allergen is safe. The nanoparticle acts as a Trojan horse, hiding the allergen in a friendly shell, thereby convincing the immune system not to attack it.
A week later, individuals with celiac disease who undertook this treatment (being injected with the nanoparticle) were fed gluten for 14 days. Results showed a remarkable tolerance to gluten and less immune inflammation response. In contrast, celiac patients without this treatment, suffered marked intestinal damage from immune response.
What is the future of celiac disease management?
As of now, only gluten avoidance is prescribed by doctors to mitigate the effects of celiac disease. With celiac disease receiving a lot of coverage in the media these days, it is expected that pathbreaking research and the use of technology may find a way to induce immune tolerance and provide comfort to celiac disease patients.
Also read: Urinary Incontinence: Types, Causes, Symptoms And Treatment
About the author:
Written by Dr Shyam Kumar on 22 November 2019
The author holds a degree in Homoeopathy with an MBA in Hospital Management and has worked across multiple disciplines including healthcare and technology. As a nature lover, he attended the world's first underwater CEO's conference to combat marine pollution.
Looking for expert tips and interesting articles on parenting? Subscribe now to our magazine. Connect with us on Facebook | Twitter | Instagram | YouTube
Join our Circles to share, discuss and learn from fellow parents and experts!

























Comments
Edit
Comment Flag
Cancel Update